Depression
2009-2010
Providing depression care in the medical home: what can we learn from attention-deficit/ hyperactivity disorder?
July 1, 2012
Garbutt JM, Leege E, Sterkel R, Gentry S, Strunk RC. Providing depression care in the medical home: what can we learn from attention-deficit/ hyperactivity disorder? Arch Pediatr Adolesc Med. 2012 Jul 1;166(7):672-3. doi: 10.1001/archpediatrics.2011.1565. PMID: 22751889; PMCID: PMC3607309.
Introduction
Although many primary care providers (PCPs) are reluctant to manage adolescent depression, they commonly provide care for children with attention deficit hyperactivity disorder (ADHD).1, 2 We sought to describe differences in care for these common diseases in order to identify opportunities to improve depression care.
Methods
PCPs from the St. Louis area completed a 29-item self-administered, mailed questionnaire (see eQuestionnaire). Questions assessed attitudes towards and behaviors regarding screening, diagnosis, and management of depressed adolescent patients. Four-point categorical scales were used to indicate agreement with attitudinal statements and confidence in delivery of depression care. Respondents also agreed or disagreed with statements about care for depression and ADHD. Washington University Human Research Protection Office approved the study.
Results
Of the respondents (100 pediatricians, 4 PNPs, 45% response), 96% wanted to improve the care they provided and 47% agreed (strongly agree or agree) that adolescent depression should be cared for in the medical home. PCPs cared for few of their depressed patients (median 5%, IQR 0–25%), although many reported frequent problems accessing psychiatry (83%) and psychotherapy (46%). Patients were identified by parental (median 50%, IQR 10–88%) or patient complaint (median 30%, IQR 0–70%); only 4% of PCPs used a validated screening tool at annual visits. PCPs lacked confidence (not very or not confident) in interpreting screening tools (43%), assessing suicide risk (37%), providing supportive counseling (60%), and monitoring treatment response (39%), and 74% suggested additional training was needed.
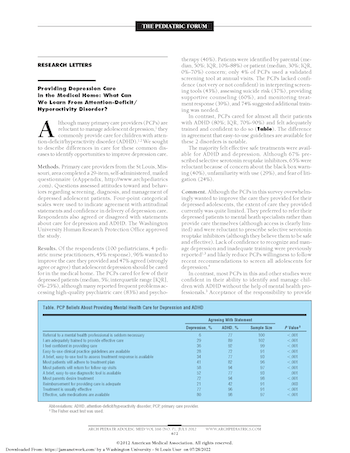
In contrast, PCPs cared for almost all their patients with ADHD (80%, IQR 70–90%) and felt adequately trained and confident to do so (Table 1). The difference in agreement that easy-to-use guidelines are available for these two disorders is notable.
The majority felt effective safe treatments were available for ADHD and depression. Although 67% prescribed selective serotonin reuptake inhibitors (SSRIs), 65% were reluctant due to concern about the Black Box warning (40%), unfamiliarity with use (29%), and fear of litigation (24%).